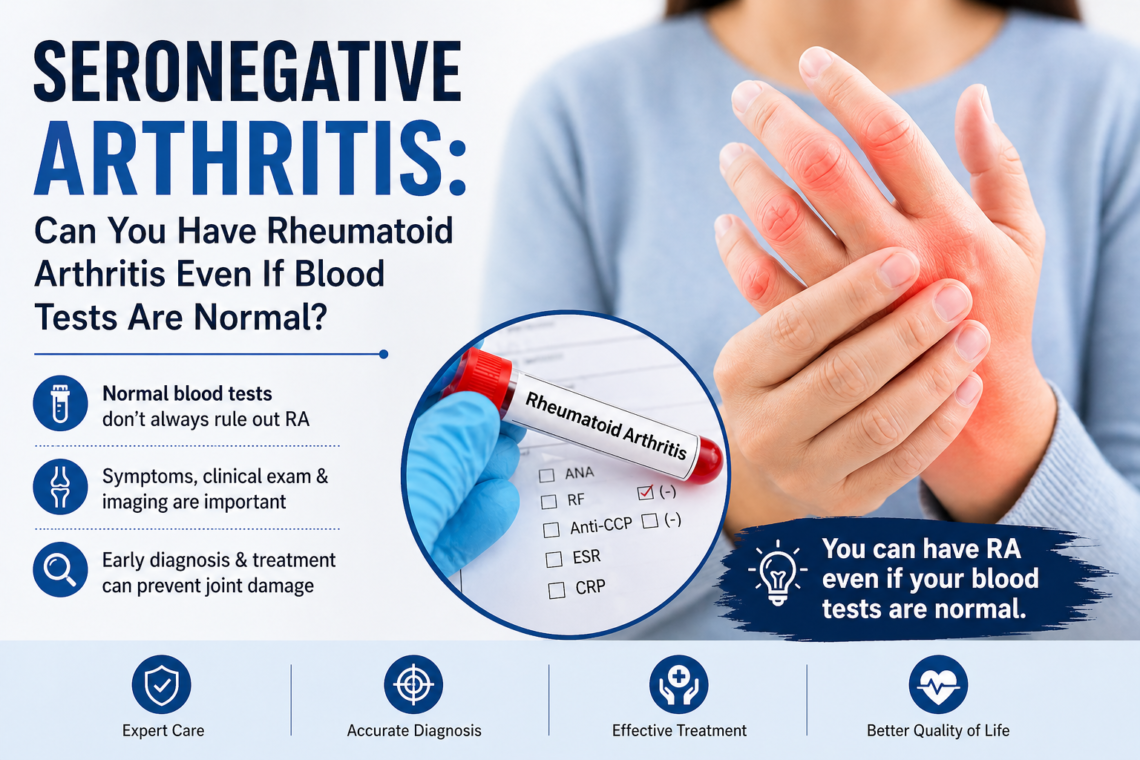
Why do your blood tests show rheumatoid factor positive when you feel perfectly fine? This question worries many people who receive unexpected lab results. Actually, rheumatoid factor has been found in up to 4% of young, healthy individuals, and it’s particularly common in older adults. A positive RF test doesn’t automatically mean rheumatoid arthritis. We’ll explain what rheumatoid factor positive meaning really is, why asymptomatic rheumatoid factor occurs, how it differs from anti-CCP testing, and when you should be concerned about your results.
What Does a Positive Rheumatoid Factor Test Mean?
What Does a Positive Rheumatoid Factor Test Mean?
Understanding Rheumatoid Factor and Its Normal Function
Rheumatoid factor is an antibody your immune system produces, but it behaves differently from the antibodies that protect you from illness. Most antibodies act as defenders, targeting germs, viruses, and other harmful invaders in your bloodstream. Rheumatoid factor, on the other hand, attacks healthy cells in your body.
Specifically, RF targets the Fc portion of immunoglobulin G (IgG), one of the most common antibodies your body makes to fight infections. Your immune system creates rheumatoid factor either by mistake or when it becomes overactive while fighting an infection. In reality, this protein doesn’t have a specific protective target like other antibodies, which is why it sometimes damages healthy tissue throughout your body.
The presence of RF isn’t always problematic. Many people have small amounts in their blood and remain perfectly healthy. RF can be part of your body’s normal response to various triggers, including bacterial toxins like lipopolysaccharides or viruses such as Epstein-Barr virus. In these cases, the RFs produced are low-affinity, transient antibodies that form immune complexes, which are then cleared by inflammatory cells. Their role could actually be protective in this context.
How RF Tests Work and What They Measure
An RF test measures the amount of rheumatoid factor in your bloodstream through a simple blood sample. A healthcare professional draws blood from a vein in your arm using a small needle, then sends the sample to a laboratory for analysis.
Labs typically measure rheumatoid factor in units per milliliter of blood (U/mL). Most assays detect IgM rheumatoid factors, although RF can occur in all immunoglobulin classes, including IgG and IgA. The test results come back either as a numerical value showing how many units of RF exist in each milliliter of your blood, or as a simple positive or negative designation.
A negative result means you have little or no rheumatoid factor in your blood. Correspondingly, a positive result indicates higher levels were detected. The test itself takes only a few minutes, though results may not return for several days.
Rheumatoid Factor Normal Range and Interpretation
A normal, healthy amount of rheumatoid factor is less than 20 units per milliliter (<20 U/mL)[7]. Some laboratories use slightly different thresholds, with results below 14 IU/mL considered normal, while others use higher cutoffs. Values may be slightly higher in older patients.
RF above 20 IU/mL is not considered enough to diagnose RA on its own, as other factors can elevate these levels. In fact, about 20% of people with confirmed RA will not have an abnormal RF test, while 5% of people who do not have RA will show elevated RF. This demonstrates why a positive result serves as a clue rather than a definitive diagnosis.
The sensitivity of RF testing in RA patients ranges from 60% to 90%, with a specificity of 85%. However, RF results are positive in less than 40% of patients with early RA. Higher RF levels generally indicate a greater likelihood of having a condition linked to rheumatoid factors, but people with rheumatoid arthritis can have little or no detectable RF. Similarly, people without rheumatoid arthritis can have substantial amounts of RF in their blood.
Your provider considers your RF levels alongside other test results, your symptoms, and your medical history to determine what’s causing any changes in your blood work.
Why Your RF Can Be Positive Without Any Symptoms
Rheumatoid Factor in Healthy Individuals
Perfectly healthy people can have elevated rheumatoid factor without any disease. In fact, RF appears in up to 4% of young, healthy individuals. Many people carry small amounts of RF in their blood and remain completely healthy throughout their lives.
Some people have high RF levels and never experience any symptoms. High amounts aren’t always a sign of a health condition. Your body might produce rheumatoid factor for no apparent reason or without a specific cause. This happens because RF can form as a normal immune response to various triggers, not just autoimmune conditions.
Most asymptomatic persons with a positive RF do not progress to RA. This bears repeating because it addresses the primary concern when you receive unexpected results. The presence of RF in your blood doesn’t predict that you’ll develop rheumatoid arthritis or any other condition. Your immune system sometimes produces these antibodies temporarily or maintains low levels indefinitely without causing tissue damage.
Age-Related Increase in Rheumatoid Factor
RF becomes increasingly common as you get older. The prevalence of RF can be as high as 14.1% in apparently healthy people aged 67-95, with a mean age of 81. This dramatic increase with age explains why many seniors receive positive results during routine blood work.
RF is also 3.5 times more common in healthy elderly subjects aged over 65 than in their younger counterparts. Your immune system changes as you age, producing more autoantibodies even when you’re healthy. These age-related changes don’t necessarily indicate disease development.
All these factors may alter the natural history of arthritis in elderly patients who have RF either in good health or in a non-arthritic presentation. Where you experience symptoms and their severity depends on where your immune system damages healthy tissue in your body.
The Timeline: When Symptoms May or May Not Develop
Some patients actually develop RF preceding the symptomatic disease. The earlier onset of RF in such patients has been associated with more severe disease. However, this represents only a subset of people with positive RF results.
Alternatively, there is a subset of patients in whom the appearance of RF follows symptoms. About 80% of all patients with rheumatoid arthritis will eventually be seropositive for rheumatoid factor, while only 40% are positive at clinical onset. This timeline variation demonstrates that RF positivity can occur at different stages or not at all.
People without rheumatoid arthritis can have substantial amounts of RF in their blood. Correspondingly, people with rheumatoid arthritis can have little or no rheumatoid factor. Your RF status today doesn’t determine your health status tomorrow.
Other Conditions That Cause Elevated Rheumatoid Factor
Other Conditions That Cause Elevated Rheumatoid Factor
Autoimmune Diseases Beyond Rheumatoid Arthritis
Rheumatoid arthritis isn’t the only autoimmune condition that triggers RF production. Several other autoimmune disorders cause elevated rheumatoid factor levels, sometimes even higher than those seen in RA patients.
Patients with Sjögren’s syndrome commonly show positive RF results. In effect, patients with primary Sjögren’s often have a positive RF test without having RA. Other rheumatic diseases that elevate RF include systemic lupus erythematosus (SLE), scleroderma, mixed connective tissue disease, and mixed cryoglobulinemia. Juvenile idiopathic arthritis also produces elevated RF in affected children.
These conditions share a common feature: uncontrolled immune system activity that becomes misdirected toward our own tissues rather than protecting us from infectious organisms. We believe some people inherit the tendency to develop these conditions, and that the diseases develop when something in the environment, perhaps an infection, stimulates the immune system to react.
Chronic Infections and RF Positivity
Chronic infections frequently cause RF elevation even when you don’t have any autoimmune disease. Hepatitis C stands out as a particularly common trigger. Hepatitis C could have very high levels of RFs, as high as 76%. Elevated rheumatoid factor levels and systemic immune activation are highly prevalent during chronic hepatitis C virus infection. This connection is so strong that it has been suggested that HCV status should be checked in all patients with increased RF levels.
The explanation lies in the nature of cryoglobulins produced during hepatitis C infection. They are cold precipitating IgM antibodies against IgG, which matches the basic definition of rheumatoid factor. By the same token, the positive rheumatoid factor could be from hepatitis C, particularly when you have arthritis and vasculitis.
Tuberculosis and subacute infective endocarditis also elevate RF. Infective endocarditis is associated with high inflammatory markers including rheumatoid factor. Actually, the latex test was positive in 45% of patients with infective endocarditis. More severe infection cases, as evidenced by duration of fever after initiation of antibiotic therapy, were more likely to develop rheumatoid factor.
Sarcoidosis and certain malignancies like primary sclerosing cholangitis also show RF elevation. Certain types of cancer, including leukemia, can cause high RF levels.
Temporary vs Persistent RF Elevation
The persistence of your elevated RF depends largely on what’s causing it. It’s not certain how a subset of chronic infections and inflammatory diseases lead to increased RF production. One explanation is chronic and persistent stimulation of the immune system by these disorders leading to a state of chronic inflammation.
Successful treatment of the underlying disorder frequently leads to the disappearance of these autoantibodies. Your RF levels can return to normal once the infection clears or the inflammatory condition resolves.
However, RF increases can be relatively stable in participants who have still not developed RA, especially in those with a combined increase of IgM and IgA RF at 74%. Unlike RA where no erosive joint changes occur, rheumatoid factor may be present in up to 50-85% of patients with certain chronic infections without causing joint damage.
Anti-CCP vs Rheumatoid Factor: Understanding the Difference
Anti-CCP vs Rheumatoid Factor: Understanding the Difference
Why Anti-CCP Is More Specific for RA
Anti-CCP stands for anti-cyclic citrullinated peptide, an autoantibody that appears early in RA development. The immune system produces anti-CCP when it mistakenly attacks certain peptides in joint linings, causing inflammation that leads to pain, swelling, and eventual joint damage. This antibody targets something fundamentally different from what RF targets, which explains why anti-CCP performs better as a diagnostic marker.
The specificity of anti-CCP reaches 95-98%, meaning it’s rarely positive in other conditions. Some studies report specificity at 96% with a positive likelihood ratio of about 14. In contrast, RF shows considerably lower specificity, ranging from 18% in some studies to 80-90% in early inflammatory arthritis. Given that RF appears in healthy individuals and numerous other conditions, anti-CCP delivers far more reliable results when diagnosing RA.
Anti-CCP antibodies may appear years before symptoms develop. Elevated levels indicate a more aggressive and destructive form of disease, serving as a marker for disease progression. In reality, anti-CCP remains negative in normal individuals, whereas RF is present in 5% of healthy people. This distinction matters when you’re trying to understand unexpected positive results without symptoms.
What It Means When RF Is Positive But Anti-CCP Is Negative
This specific combination suggests you’re unlikely to have RA, though clinical evaluation remains necessary. Studies show that 24.2% of anti-CCP-negative patients tested positive for RF. The interpretation changes based on your clinical presentation and other test results.
When anti-CCP is positive but RF is negative, you may be in the early stages of RA or could develop it in the future. This pattern appears in approximately 7.3% of cases. Correspondingly, when both tests come back negative, RA becomes highly unlikely, though seronegative RA still requires clinical evaluation to rule out.
Combining Both Tests for Better Accuracy
Doctors order both tests together, along with C-reactive protein and erythrocyte sedimentation rate, for complete diagnosis. Double positivity for RF and anti-CCP notably increases the positive likelihood ratio of RA. When both tests show positive results, you probably have rheumatoid arthritis, occurring in about 11.3% of cases.
Testing for both RF and anti-CCP is ideal for diagnosis. If testing for only one marker, anti-CCP is most recommended. The combined approach provides more accurate diagnosis than using RF testing results alone. Studies have shown that anti-CCP is positive even in RA patients who are RF negative.
When to Worry About Your Positive Rheumatoid Factor and What to Do Next
Warning Signs That Require Medical Attention
Joint symptoms warrant immediate medical attention. Pain, swelling, stiffness, and tenderness in more than one joint signal potential rheumatoid arthritis development. Morning stiffness or pain after sitting for long periods indicates inflammatory arthritis. RA typically affects joints on both sides of your body, so if one hand or knee hurts, watch the other.
Increased joint pain and swelling, new joint deformities, or feeling more tired and stiff for longer periods suggest your condition may be worsening. Fatigue, weakness, and low-grade fever accompanying joint problems require evaluation. Hard bumps under your skin near joints, called rheumatoid nodules, are red flags.
Patients with inflammatory joint disease should be referred to a rheumatology subspecialist, especially if symptoms last more than six weeks.
When to Repeat or Further Investigate Your Test Results
Inappropriate repeat testing of RF is common, and the results only rarely change. Patients who have clearly tested positive for RF or anti-CCP should not be retested routinely. RF and anti-CCP have no role in assessing disease activity.
Your clinician may check your RF level again if you were initially negative, but ongoing monitoring is based on symptoms, inflammation markers, and imaging. However, most asymptomatic persons with a positive RF do not progress to RA.
Do You Need Treatment If RF Is Positive But You Have No Joint Pain?
Treatment depends on the underlying cause. Without symptoms, you don’t need treatment for RA. Early diagnosis and effective treatment are important only when symptoms develop.
Working With Your Doctor to Monitor Your Condition
Track any new or worsening symptoms and share details with your clinician. This helps them adjust your treatment plan if needed. Regular monitoring focuses on symptom development rather than repeatedly checking RF levels.
Conclusion
We’ve demystified what rheumatoid factor positive really means when you have no symptoms. By and large, your positive RF test doesn’t predict rheumatoid arthritis development, particularly if your anti-CCP remains negative. Many healthy people carry RF in their blood without ever experiencing problems. Age-related increases, chronic infections, and various autoimmune conditions can all elevate your RF levels.
Focus on your symptoms rather than the numbers. You should worry only on the condition that you develop joint pain, swelling, or morning stiffness affecting multiple joints. Work with your doctor to monitor your health, but remember that most asymptomatic people with positive RF never progress to disease. Your blood test is just one piece of your overall health picture.
Key Takeaways
Understanding your positive rheumatoid factor test without symptoms can ease unnecessary worry and guide appropriate next steps.
• Positive RF doesn’t equal rheumatoid arthritis – Up to 4% of healthy young people and 14% of elderly individuals have elevated RF without any disease
• Anti-CCP testing is more reliable – Anti-CCP has 95-98% specificity for RA compared to RF’s lower accuracy, making it the better diagnostic marker
• Multiple conditions cause RF elevation – Chronic infections like hepatitis C, autoimmune diseases, and even normal aging can trigger positive results
• Symptoms matter more than numbers – Focus on joint pain, swelling, and morning stiffness rather than RF levels; most asymptomatic people never develop RA
• Monitor symptoms, not RF levels – Routine retesting of positive RF is unnecessary; work with your doctor to watch for actual disease signs instead
The key insight is that RF positivity without symptoms rarely indicates future disease development, especially when combined with negative anti-CCP results and absence of joint inflammation.
FAQs
Q1. Is it possible to have elevated rheumatoid factor without experiencing any symptoms?
Yes, it’s entirely possible to have high RF levels without any symptoms. Many healthy individuals have elevated rheumatoid factor in their blood and never develop any health problems. Up to 4% of young, healthy people and as many as 14% of elderly individuals have positive RF tests without any disease. The presence of RF alone doesn’t predict that you’ll develop rheumatoid arthritis or other conditions.
Q2. What does it mean if my rheumatoid factor is positive but my anti-CCP test is negative?
When RF is positive but anti-CCP is negative, it generally suggests you’re unlikely to have rheumatoid arthritis, though clinical evaluation is still important. Anti-CCP is much more specific for RA (95-98% specificity) compared to RF, which can be elevated in many other conditions including chronic infections, other autoimmune diseases, and normal aging. This combination is relatively common and doesn’t necessarily indicate disease.
Q3. How common is rheumatoid factor positivity in people with confirmed rheumatoid arthritis?
Approximately 60-80% of people with RA will have positive RF during the course of their disease. However, only about 40% of patients with early RA test positive for RF. This means that RF can be absent even when someone has rheumatoid arthritis, and conversely, it can be present in people who don’t have the disease, which is why doctors use it alongside other tests and clinical symptoms for diagnosis.
Q4. What symptoms should prompt me to see a doctor if I have a positive rheumatoid factor?
You should seek medical attention if you develop joint pain, swelling, stiffness, or tenderness affecting multiple joints, especially on both sides of your body. Morning stiffness lasting more than 30 minutes, fatigue, low-grade fever, or hard bumps under your skin near joints are warning signs. If joint symptoms persist for more than six weeks, a referral to a rheumatologist is recommended.
Q5. Besides rheumatoid arthritis, what other conditions can cause elevated rheumatoid factor?
Many conditions can elevate RF levels, including chronic infections like hepatitis C (which shows positive RF in up to 76% of cases), tuberculosis, and infective endocarditis. Other autoimmune diseases such as Sjögren’s syndrome, lupus, and scleroderma also cause RF elevation. Even certain cancers and normal aging can increase RF levels without indicating rheumatoid arthritis.
Q6. What does a positive rheumatoid factor (RF) mean?
A positive RF means that a specific antibody is detected in your blood. While it is commonly associated with Rheumatoid Arthritis, it is not exclusive to it. Many people can have a positive RF without having any disease.
Q7. Can I have a positive RF and still be completely healthy?
Yes. A significant number of people, especially older adults, may have a positive RF without any symptoms or illness. In such cases, it may not have clinical significance.
Q8. Does a positive RF always mean I will develop rheumatoid arthritis?
No. A positive RF does not guarantee that you will develop rheumatoid arthritis. It is just one piece of the puzzle and must be interpreted along with symptoms and other tests.
Q9. What other conditions can cause a positive RF?
RF can also be elevated in other conditions such as:
- Chronic infections (like hepatitis or tuberculosis)
- Other autoimmune diseases like Systemic Lupus Erythematosus
- Certain lung or liver diseases
Q10. What is the difference between RF and anti-CCP?
RF is less specific, meaning it can be positive in multiple conditions. Anti-CCP (anti-cyclic citrullinated peptide) is more specific for rheumatoid arthritis and helps confirm the diagnosis when symptoms are present.
Q11. Should I start treatment if my RF is positive but I have no symptoms?
No treatment is needed based on RF alone. Treatment decisions are made only if you have symptoms like joint pain, swelling, or stiffness.
Q12. Can rheumatoid factor levels go back to normal?
Yes, RF levels can fluctuate and may even return to normal over time, especially if they were elevated due to a temporary cause like an infection.
Q13. When should I be concerned about a positive RF?
You should consult a doctor if you develop:
- Persistent joint pain or swelling
- Morning stiffness lasting more than 30 minutes
- Fatigue or unexplained weakness
Q14. Do I need further tests if my RF is positive?If you have no symptoms, often no immediate action is required. However, your doctor may advise:
- Anti-CCP test
- ESR/CRP (inflammation markers)
- Clinical follow-up over time
Q15. How often should I repeat the RF test?
Routine repetition is usually not necessary if you are asymptomatic. Follow-up testing is guided by clinical changes rather than lab numbers alone.
Consult Dr. Manu Mengi for all types of joint pain and orthopedic problems. A Top orthopedic doctor in Chandigarh, he provides care for bone and joint.

Dr. Manu Mengi is a best orthopedic doctor in Mohali, specializing in joint pain, arthritis, and sports injuries. With qualifications in orthopedics and advanced training in joint replacement, he provides effective care for bone and joint conditions, helping patients improve mobility and manage pain with the right treatment approach.