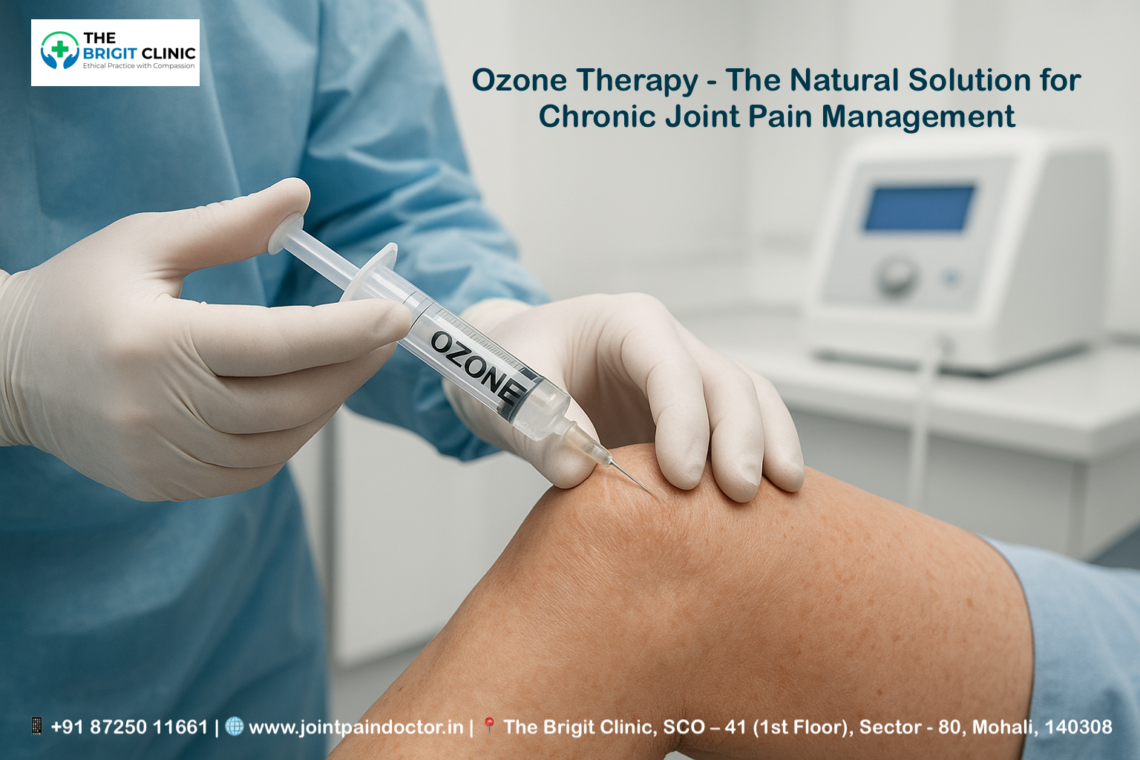
Are you struggling with persistent joint pain? Ozone Infusion Therapy has been studied and utilised for more than a century, offering a potential alternative approach to managing chronic joint discomfort. Despite the U.S. Food and Drug Administration (FDA) issuing a warning against using ozone therapy in 2019, this controversial alternative medicine practice continues to attract attention for its possible health benefits.
Although currently not FDA-approved as a medical treatment, ozone therapy demonstrates considerable therapeutic applications in the management of musculoskeletal disorders, including osteoarthritis and chronic pain syndromes. Research has shown limited but promising evidence that this treatment might help with various conditions, such as arthritis and diabetes. For example, its anti-inflammatory properties and potential to improve joint mobility make it an intriguing option for those seeking relief from joint pain. However, it’s important to note that studies have raised concerns regarding its potential toxicity, emphasising the need for stringent administration protocols to ensure safety.
In this comprehensive guide, you’ll discover what ozone therapy is, how it works for joint pain, its potential benefits, and what scientific evidence says about its effectiveness. You’ll also learn about important safety considerations to help you make an informed decision about whether this alternative treatment might be right for your joint health needs.
Considering advanced pain management solutions? Consult with the Best Orthopaedics Doctors in Mohali at The Brigit Clinic to discuss if ozone therapy is a suitable option for your joint health. Call +91 87250 11661 to book an appointment.
What is Ozone Therapy and How Does It Work?
Ozone gas consists of three oxygen atoms (O3) arranged in an unstable molecular structure, making it significantly different from the oxygen we breathe (O2). Discovered in the 1840s, ozone’s potential as more than just another atmospheric gas has evolved considerably over time. Its unique properties and therapeutic applications have made ozone therapy an intriguing option for those seeking alternative approaches to managing joint conditions.
Understanding the O3 molecule
The O3 molecule has a bent structure with an O–O–O angle of 116.78° and O–O distances of 127.2 pm. This unstable arrangement creates what scientists call “mesomeric states,” which contribute to ozone’s highly reactive nature. Unlike stable oxygen, ozone is pale blue as a gas, turns dark blue when condensed into liquid form at extremely low temperatures, and becomes violet-black when solidified.
Ozone’s instability is both a challenge and an advantage in medical applications. Due to its unstable molecular configuration, ozone readily dissolves in water and reacts quickly with biological components. This high reactivity makes it difficult to maintain concentrated forms, as ozone rapidly undergoes transient reactions with itself or water. Furthermore, ozone is approximately 10 times more soluble in water than regular oxygen, enabling it to interact effectively with body tissues and fluids.
How ozone interacts with the body
When introduced to the body, ozone functions similarly to a prodrug—it reacts with molecules to create more active substances that trigger a cascade of biological responses. Upon contact with the aqueous component of plasma, ozone dissolves and reacts with polyunsaturated fatty acids (PUFAs) and water to form hydrogen peroxide (H2O2) and lipid ozonation products (LOPs).
This moderate oxidative stress initiates several important mechanisms:
- Activation of antioxidant systems – Ozone stimulates the transcription factor Nrf2, which activates antioxidant response elements (ARE). This leads to increased production of antioxidant enzymes such as superoxide dismutase (SOD), glutathione peroxidase (GPx), and catalase (CAT).
- Enhanced oxygen metabolism – Ozone increases the transmembrane flow of oxygen and makes the mitochondrial respiratory chain more efficient. In red blood cells, it boosts glycolysis, raising ATP and 2,3-diphosphoglycerate levels, which allows haemoglobin to release oxygen more readily to tissues.
- Anti-inflammatory effects – Through modulation of inflammatory mediators, ozone reduces prostaglandin synthesis and decreases joint oxidative stress. It also activates key signalling pathways that support tissue regeneration and repair.
The therapeutic principle resembles hormesis, where low-dose exposure to a stressor triggers beneficial adaptive responses. Much like exercise, moderate ozone exposure can be beneficial, whereas excessive exposure can be harmful. This controlled oxidative stress preconditions cells to become more resilient against future oxidative damage, a phenomenon known as “oxidative preconditioning”.
Why ozone is considered for joint pain
Joint pain, particularly in conditions like osteoarthritis, is characterised by inflammation, oxidative stress, and tissue degeneration. Ozone therapy addresses these fundamental aspects through multiple mechanisms, making it potentially valuable for managing joint conditions.
Firstly, ozone’s ability to reduce inflammation helps mitigate the inflammatory response that drives joint pain and degeneration. Additionally, by improving tissue oxygenation and cellular metabolism, ozone therapy may support the repair processes within damaged joint tissues.
The anti-inflammatory effects are especially relevant in knee osteoarthritis, where ozone can inhibit inflammatory mediators like IL-1β and Nerve Growth Factor (NGF), which contribute significantly to pain sensations. Moreover, ozone’s capacity to stimulate antioxidant systems helps neutralise the harmful free radicals that accumulate in inflamed joints.
Clinical applications further demonstrate ozone’s versatility for joint conditions through various administration methods. Ozone can be delivered via intra-articular injections directly into affected joints, or through systemic approaches like major autohemotherapy (MAH), where blood is drawn, exposed to ozone, and reinfused. These delivery methods ensure that ozone’s therapeutic benefits reach the target areas effectively, potentially offering relief from chronic joint pain with minimal side effects when administered according to precise protocols.
Understanding the science behind treatments is key. Our Top Orthopaedic Doctors in Mohali SAS Nagar at The Brigit Clinic are experts in advanced therapies and can provide a clear, personalised explanation for your condition. Visit us in Sector 80, Mohali (Get Directions), to learn more.
How Ozone Therapy is Administered for Joint Pain
Medical professionals employ various methods to deliver ozone therapy for joint pain, each tailored to specific conditions and patient needs. The route of administration significantly impacts how ozone interacts with joint tissues and the resulting therapeutic effects.
Ozone injection therapy explained
Joint pain treatment typically involves direct ozone administration through several approaches. Practitioners primarily use intra-articular injections, where a mixture of oxygen-ozone (95-96% oxygen and 4-5% ozone) is delivered directly into the affected joint cavity. For knee osteoarthritis, a common protocol involves injecting 20 ml of ozone-oxygen mixture at a concentration of 20 μg/ml.
Periarticular injections target tissues surrounding the joint, while paravertebral injections help with spine-related pain conditions. These targeted approaches enable ozone to directly influence the biochemical environment of the joint, addressing inflammation at its source.
In cases like frozen shoulder or hip bursitis, ozone infiltration can significantly reduce both pain and inflammation through peritrochanteric routes. Before the procedure, local anaesthetics such as 1% lidocaine are often applied to minimise discomfort.
Topical and systemic applications
Beyond injections, practitioners utilise several external and whole-body approaches. Topical applications involve exposing affected areas to ozone gas under protective coverings (sometimes called “ozone sauna”) or applying ozonised solutions directly to the skin. These methods are particularly valuable for addressing superficial joint issues.
Systemic ozone delivery can occur through insufflation techniques, where ozone gas is introduced into body cavities. This approach allows ozone to be absorbed through mucous membranes, creating whole-body effects that complement localised treatments.
Autohemotherapy and IV methods
Autohemotherapy stands out as one of the most extensively studied systemic ozone administration methods. During major autohemotherapy (MAH), approximately 200 ml of blood is withdrawn from the patient, mixed with 40 ml of medical ozone at a concentration of 30 μg/ml, and then reinfused within 15 minutes. This procedure is typically performed three times weekly for two weeks.
Minor autohemotherapy involves smaller blood volumes (60-80 ml) mixed with ozone and then injected intramuscularly into the buttock. IV ozone therapy follows similar principles to other infusions, with ozone-enriched blood returning to circulation via drip methods.
A modern advancement called hyperbaric ozone/oxygen treatment modifies traditional autohemotherapy to deliver larger ozone quantities in fewer sessions. This approach can significantly reduce the number of treatments needed while maximising therapeutic benefits.
Safety protocols during administration
Proper safety measures are essential during ozone therapy. Fundamentally, ozone should never be inhaled, as this can cause severe lung irritation and fluid buildup. Medical-grade equipment with precise concentration controls and sterile application techniques is mandatory.
Qualified healthcare professionals must administer treatments in controlled clinical environments. The oxygen-ozone mixture should be produced through specialised medical generators that ensure precise concentrations. Practitioners should follow established protocols, with ozone concentrations for systemic therapy typically ranging between 10-40 μg/ml.
Most importantly, each treatment plan should be individually tailored. As no two patients are alike, dosage and administration protocols require personalisation based on specific conditions and responses.
The correct administration technique is critical for safety and effectiveness. Ensure you are in expert hands. Schedule a consultation with an Orthopedic Doctor in Mohali from our team to discuss the best administration method for you.
Ozone Therapy Benefits for Chronic Joint Conditions
Research demonstrates that Ozone Infusion Therapy offers multiple benefits for patients suffering from chronic joint conditions. Studies reveal its effectiveness across various joint disorders, making it an increasingly popular alternative treatment option.
Ozone therapy for arthritis and osteoarthritis
Clinical studies show that intra-articular ozone injections can effectively alleviate pain and inhibit cartilage degeneration in osteoarthritis (OA). OA affects over 346 million people globally and is characterised by inflammation in cartilage and synovium. In a study of patients with knee osteoarthritis, approximately 50% improvement in health status was observed after just five weekly sessions of ozone therapy. Notably, treatments using concentrations between 20-30 μg/mL have demonstrated significant pain reduction and functional improvement over six-month periods.
Reducing inflammation and oxidative stress
The therapeutic effects of ozone stem from its ability to modulate inflammation through multiple pathways. Ozone decreases the production of pro-inflammatory cytokines—particularly IL-6, IL-1β, and TNF-α—which are primarily responsible for cartilage degradation. In fact, studies have demonstrated that ozone therapy reduces these inflammatory markers at 1, 2, and 6 months after treatment, with effects more stable than steroid injections.
Consequently, ozone inhibits the NF-κB pathway while enhancing the Nrf2 pathway, which generates antioxidant response elements, including superoxide dismutase and glutathione peroxidase. This dual action creates what scientists call “oxidative preconditioning,” preparing cells to better resist future oxidative damage.
Improving joint flexibility and mobility
Patients receiving ozone treatment experience significant improvements in joint function and mobility. Clinical trials report notable increases in Lysholm scores (measuring knee function) alongside decreases in WOMAC and VAS pain scores following treatment. Essentially, these improvements occur because ozone enhances oxygen metabolism and blood circulation to affected joints.
Supporting cartilage and ligament healing
Ozone therapy actively supports tissue repair mechanisms. Research shows it reduces the release of matrix metalloproteinases (MMPs) that degrade cartilage while simultaneously stimulating chondrocytes to facilitate the synthesis of proteoglycans, glycosaminoglycans, and collagen. This balanced approach helps repair damaged joint structures and potentially slows disease progression.
Enhancing immune response in chronic disease
Beyond local effects, ozone therapy provides systemic immune benefits. It activates the immune system by functioning like an antioxidant or anti-inflammatory agent. Studies reveal that ozone can regulate immune functions, particularly enhancing macrophage activity crucial for immune reactions. Furthermore, ozone’s ability to improve liver mitochondrial function and modulate antioxidant responses may contribute to its systemic therapeutic effects.
These multifaceted benefits make Ozone Therapy worthy of consideration for those seeking alternative approaches to managing chronic joint conditions.
Ready to explore the benefits of ozone therapy for your arthritis or joint pain? Talk to the Best Orthopedic Surgeon in Mohali at The Brigit Clinic to see if you are a candidate. Find relief and improve your mobility today!
Scientific Evidence and Effectiveness in Orthopaedic Use
Scientific research increasingly supports the effectiveness of Ozone Infusion Therapy across various orthopaedic applications. Multiple clinical trials highlight its potential as both a primary and complementary treatment option.
Clinical trials on ozone therapy for knee osteoarthritis
Recent systematic reviews examining ozone therapy for knee osteoarthritis (KOA) revealed statistically significant effects in pain reduction compared to placebo groups. Intra-articular ozone at concentrations of 20-30 μg/mL demonstrated substantial improvements in both pain management and functional mobility over six-month periods. Remarkably, one double-blind randomised trial found that both 20 μg/mL and 40 μg/mL doses effectively reduced pain without significant differences between concentrations, suggesting a threshold effect where lower doses sufficiently activate therapeutic pathways.
Ozone therapy for spinal arthritis and back pain
For back pain treatment, ozone therapy has shown success rates of 70-80% in patients with disk herniation. Intramuscular paravertebral ozone injections produced Visual Analogue Scale (VAS) reductions in 79% of patients while simultaneously improving Oswestry Disability Index scores in nearly all cases. Interestingly, these treatments can be performed without computed tomography guidance or an anesthesiologist’s support, making them accessible options for many practitioners.
Post-surgical recovery and pain management
Ozone therapy shows promise in post-surgical recovery scenarios. Indeed, in one preliminary study involving patients with methicillin-resistant Staphylococcus aureus (MRSA) infections following surgery, ozone therapy substantially reduced bacterial counts by at least 2 logs CFU/mL (p = 0.00093097). Subsequently, inflammation markers decreased dramatically—C-reactive protein dropped by 98.95% (p = 0.0007) and erythrocyte sedimentation rate by 75.78% (p = 0.0002).
Comparisons with traditional treatments
When compared with conventional therapies, ozone shows comparable or superior results in several studies. In comparison with hyaluronic acid for KOA treatment, both treatments significantly improved pain, stiffness, and function at 1, 3, and 6-month follow-ups with no significant differences between groups. Nevertheless, ozone demonstrated superiority over corticosteroid injections in longer-term outcomes—at 12 weeks, ozone produced significantly better pain reduction (mean difference = 3.9, p < 0.01). Correspondingly, clinical studies found ozone marginally favoured over periradicular steroid infiltrations for medium and long-term pain management in back pain patients.
Evidence-based practice is our priority. Our Orthopedic Doctors in Mohali stay updated with the latest research to offer you the most effective treatments. Contact us to discuss the scientific evidence supporting your care plan.
Risks, Side Effects, and Regulatory Considerations
Though ozone therapy shows promise for joint pain, understanding its risks is vital for patient safety. Several adverse effects have been documented, ranging from mild to severe.
Potential side effects and contraindications
Air embolism represents a serious risk during IV ozone therapy, potentially causing stroke or heart attack. Patients commonly experience discomfort, cramping, and occasional flu-like symptoms (Herxheimer reaction) as the body responds to treatment. Altogether, contraindications include glucose-6-phosphate dehydrogenase deficiency, pregnancy, hyperthyroidism, thrombocytopenia, cardiovascular instability, and recent myocardial infarction. Patients taking ACE inhibitors should exercise caution, as sudden hypotension may occur.
Why is inhalation dangerous?
Primarily, ozone should never be inhaled. Even brief exposure to small amounts can cause severe lung damage. Initially, patients might experience burning eyes, coughing, nausea, or headaches, alongside throat irritation and chest tightness. Over time, inhaled ozone may lead to chronic conditions like asthma or COPD.
FDA stance and lack of standardisation
The FDA prohibits ozone use “in any medical condition for which there is no proof of safety and effectiveness”. Rather than approving it, the FDA has prosecuted individuals selling ozone therapy products as medical cures. Currently, no standardised protocols exist—concentrations, dosages, and administration methods vary widely across practitioners.
How to find a qualified provider
Before treatment, verify that the provider uses medical-grade equipment with precise concentration controls. Qualified practitioners should follow established protocols with ozone concentrations typically between 10-40 μg/ml for systemic therapy. Additionally, they must be trained in emergency procedures and have equipment like an Ambu, medical oxygen, and emergency medications.
Your safety is non-negotiable. It is essential to choose a qualified and experienced provider. Trust the Top Orthopedics Doctor in Mohali at The Brigit Clinic, where stringent safety protocols are always followed. Call us to address any concerns.
Conclusion
Ozone therapy represents a fascinating alternative approach for those suffering from chronic joint pain. Throughout this article, we’ve explored how this unique three-atom oxygen molecule works within the body to potentially reduce inflammation, combat oxidative stress, and support tissue healing. Although not FDA-approved, research suggests ozone therapy may offer significant benefits for conditions like osteoarthritis through various delivery methods such as intra-articular injections, topical applications, and autohemotherapy.
Scientific evidence increasingly supports ozone therapy’s effectiveness for joint conditions. Clinical trials demonstrate promising results for knee osteoarthritis patients, with many experiencing substantial pain reduction and improved mobility. Similarly, back pain sufferers have shown positive outcomes comparable to traditional treatments in several studies. Nevertheless, these benefits must be weighed against potential risks.
Safety considerations remain paramount when exploring ozone therapy. Under no circumstances should you inhale ozone gas, as this can cause severe respiratory damage. Additionally, treatment should only be sought from qualified practitioners using medical-grade equipment. While the FDA has not approved ozone for medical treatment, many patients still pursue this alternative therapy under proper medical supervision.
Before trying ozone therapy, carefully consider your specific health condition, consult with healthcare providers familiar with both conventional and alternative approaches, and thoroughly research qualified practitioners. Ultimately, ozone therapy offers an intriguing option that might complement traditional joint pain management strategies for some individuals. The decision rests with you and your healthcare team to determine if this alternative treatment aligns with your joint health needs and overall wellness goals.
Key Takeaways
Ozone therapy offers a promising alternative approach to chronic joint pain management through multiple therapeutic mechanisms, though it requires careful consideration of safety protocols and regulatory status.
• Ozone therapy reduces joint inflammation by decreasing pro-inflammatory cytokines (IL-6, IL-1β, TNF-α) and activating antioxidant pathways for tissue repair.
• Clinical studies show 50% improvement in knee osteoarthritis patients after five weekly sessions, with effects lasting up to six months.
• Multiple delivery methods exist, including intra-articular injections (20-30 μg/mL), autohemotherapy, and topical applications for targeted treatment.
• Never inhale ozone gas as it causes severe lung damage; only seek treatment from qualified practitioners using medical-grade equipment.
• FDA has not approved ozone therapy for medical use, emphasising the importance of consulting healthcare providers before pursuing treatment.
While research demonstrates ozone therapy’s potential for managing chronic joint conditions like arthritis and osteoarthritis, patients must weigh promising clinical outcomes against safety risks and regulatory considerations. The therapy’s ability to support cartilage healing and improve joint mobility makes it an intriguing complement to traditional treatments when administered properly by qualified professionals.
FAQs
Q1. What is ozone therapy, and how does it work for joint pain?
A1. Ozone therapy is a treatment that uses medical-grade ozone gas to reduce inflammation and promote healing in joints. It works by stimulating the body’s antioxidant systems, improving oxygen metabolism, and modulating inflammatory responses in affected areas.
Q2. How is ozone therapy administered for joint conditions?
A2. Ozone therapy can be administered through various methods, including intra-articular injections directly into the affected joint, autohemotherapy (where blood is mixed with ozone and reinfused), and topical applications. The specific method depends on the condition being treated and the practitioner’s approach.
Q3. What are the potential benefits of ozone therapy for chronic joint pain?
A3. Potential benefits include reduced inflammation, improved joint mobility, decreased pain, enhanced tissue repair, and better overall joint function. Some patients report significant improvements in conditions like osteoarthritis and chronic back pain after undergoing ozone therapy.
Q4. Are there any risks or side effects associated with ozone therapy?
A4. While generally considered safe when administered properly, ozone therapy can have side effects such as temporary discomfort, flu-like symptoms, and, in rare cases, more serious complications like air embolism. It’s crucial never to inhale ozone gas as it can cause severe lung damage.
About Dr. Manu Mengi – Best Orthopaedic Doctors in Mohali
Dr. Manu Mengi is a distinguished name in orthopaedics, renowned as one of the Best Orthopaedic Doctors in Mohali. Practicing at The Brigit Clinic in Sector 80, Mohali, Dr. Mengi is committed to providing compassionate and comprehensive care for a wide range of joint, bone, and musculoskeletal conditions. With a patient-centric approach, he combines advanced treatments like ozone therapy with proven surgical and non-surgical interventions to develop personalised recovery plans. If you are seeking expert guidance for chronic joint pain from a trusted Orthopaedic Doctor in Mohali, schedule a consultation with Dr. Manu Mengi to take a decisive step towards a pain-free, active life.
#OzoneTherapy #JointPainRelief #ChronicPainManagement #MohaliOrtho #BestOrthopedicSurgeonInMohali #DrManuMengi #TheBrigitClinic #OrthopedicCare #NaturalPainRelief #OzoneTreatment #ArthritisRelief #Osteoarthritis #HealthTech #AlternativeMedicine #MohaliDoctors

Dr. Manu Mengi is a best orthopedic doctor in Mohali, specializing in joint pain, arthritis, and sports injuries. With qualifications in orthopedics and advanced training in joint replacement, he provides effective care for bone and joint conditions, helping patients improve mobility and manage pain with the right treatment approach.