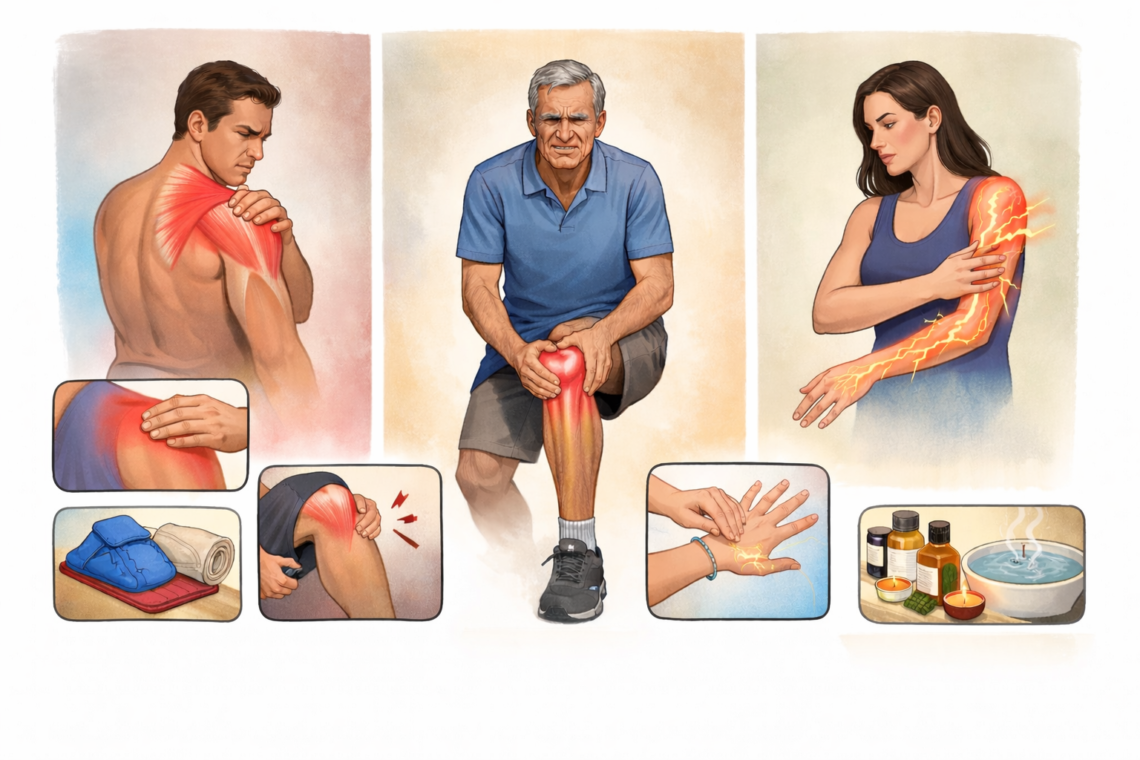
Figuring out if your pain is coming from muscle, joint, or nerve can feel confusing when you’re dealing with discomfort. Most daily aches come from muscles or joints, while true nerve pain is less common but easier to recognize once you know the signs. Pain is our body’s way of signaling that something isn’t right, and treating it incorrectly can prolong discomfort or even worsen the condition. In this guide, I’ll walk you through the key differences between muscle pain vs joint pain vs nerve pain and show you simple at-home tests to identify your pain source.
Understanding the Three Types of Pain
Before you can identify your pain source, you need to understand what makes each type distinct. Each category has unique characteristics that reveal what’s happening beneath your skin.
What is muscle pain (myalgia)?
Muscle pain shows up as deep discomfort within your muscle tissue. You’ll typically feel it as a dull, achy sensation that you can pinpoint to a specific spot. When I press on the affected area, it feels tender and sore to the touch.
This type of pain usually appears after physical activity. You might experience it following a long day of yard work, a new workout routine, or even after sleeping in an awkward position. The pain often feels like a muscle pull, presenting as either sharp or dull aching sensations.
Muscle pain can be localized to one specific area, or it can spread throughout your body in cases of systemic conditions like the flu. If you’re dealing with chronic muscle pain, the discomfort persists whether you’re moving or staying still. In addition to the pain itself, the affected muscles often become swollen and feel stiff when you try to use them.
What is joint pain?
Joint pain occurs at the points where two or more bones come together. Your hips, knees, spine, hands, and feet are common locations for joint discomfort.
The sensation differs from muscle pain in how it feels. You might describe it as stiff, achy, or sore, but many people report additional sensations like burning, throbbing, or a “grating” feeling inside the joint. This pain can be constant, or it might come and go throughout your day.
One telltale pattern with joint pain is morning stiffness. Your joints feel particularly rigid when you first wake up, but they tend to loosen up as you move and go about your activities. On the other hand, too much activity can make the pain worse. Joint pain affects your ability to perform basic tasks like climbing stairs, writing, or carrying objects.
What is nerve pain (neuropathy)?
Nerve pain happens when your nervous system malfunctions or sustains damage. Your nervous system includes peripheral nerves that spread throughout your body to your arms, legs, fingers, and toes, as well as your central nervous system consisting of your spinal cord and brain.
When nerve fibers get damaged, they send incorrect signals to your pain centers. About 30% of neuropathy cases occur due to diabetes, but hundreds of other conditions can cause it.
Nerve pain feels distinctly different from muscle or joint pain. Patients describe it as burning, stabbing, or electric shock-like sensations. You might experience tingling, numbness, or a “pins and needles” feeling. In contrast to localized muscle pain, nerve pain often travels. You could feel it shooting down your leg even though the problem starts in your back.
Nerve pain can include several specific symptoms:
- Allodynia: Normally painless stimuli like cold, light pressure, or brushing against your skin causes pain
- Hyperalgesia: Normally painful stimuli like heat or pinpricks produce an extreme or increased pain sensation
- Hypoalgesia: A normally painful stimulus results in a decreased pain response
- Dysesthesia: Unexpected sensations that feel strange, unpleasant, or painful
- Spontaneous pain: Pain that happens without any apparent reason or trigger
This type of pain typically doesn’t improve with simple rest. It often comes with numbness or weakness in the affected area, which are red flags that distinguish it from other pain types. The chronic nature of nerve pain sets it apart, as damaged tissue often leads to ongoing, constant discomfort.
How to Tell the Difference: Key Signs and Symptoms
Once you understand the basics of each pain type, the next step is learning how to distinguish between them through observable characteristics. The way your pain feels, where it appears, and how it responds to different triggers tells you which tissue is causing the problem.
Pain sensation: sharp vs dull pain meaning
The quality of your pain sensation reveals important clues about its source. Sharp pain travels through myelinated A-delta fibers that insulate the nerve, allowing signals to move faster and creating immediate, easily identifiable sensations. Dull pain moves through unmyelinated C fibers that transmit messages more slowly, spreading over a larger area and producing aches that are difficult to pinpoint.
Muscle and joint pain typically presents as dull or achy feelings. You might describe it as pressure or heaviness rather than something stabbing. Nerve pain feels distinctly different. Patients describe it as burning, tingling, shooting, or electric shock-like sensations. If your pain feels like electricity running through your body or a burning sensation without any visible injury, nerve damage is the likely culprit.
Location: radiating pain vs localized pain
Pain location patterns provide one of the clearest ways to identify your pain source. Localized pain stays confined to a particular area of your body. When you sprain your ankle or strain a muscle, the pain remains at the injury site. This somatic pain results from inflammation releasing chemical messengers that activate local pain receptors.
Radiating pain behaves completely differently. It travels from one spot to other areas following specific nerve pathways. Sciatica demonstrates this perfectly when pain starts in your lower back but shoots down your leg. Radicular pain occurs when spinal nerves become compressed or inflamed, sending sharp, shooting sensations along the nerve’s route. If your pain follows a pathway or moves from your back down your arm or leg, you’re dealing with nerve involvement.
Response to touch and pressure
How your pain responds to touch distinguishes nerve issues from muscle or joint problems. Muscle pain increases when I press directly on the affected area. The tender spot reproduces your discomfort.
Nerve pain creates unusual touch responses. Allodynia makes normally painless stimuli like light pressure or fabric brushing against your skin feel painful. Inflammation can cause tactile allodynia where touch becomes hypersensitive. Similarly, hyperalgesia amplifies normally painful sensations beyond what you’d expect.
Movement patterns and timing
Movement affects each pain type differently. Muscle pain often feels sharp with movement but becomes a constant dull ache at rest. Joint pain typically presents with morning stiffness that improves as you move throughout your day.
Nerve pain shows distinct mechanical provocation patterns. Tests that move, load, or compress neural tissue trigger symptoms. Your pain might worsen when you bend, and physical exertion can introduce additional discomfort. Night pain that disrupts your sleep points toward nerve involvement.
Tingling numbness causes pain type
Tingling and numbness almost always indicate nerve problems rather than muscle or joint issues. Peripheral neuropathy creates gradual numbness, prickling, or tingling that typically starts in your feet or hands and spreads upward into your legs and arms. These sensations accompany nerve pain but rarely appear with muscle or joint conditions.
You might experience pins-and-needles feelings, weakness, or paralysis alongside the numbness. Pain during activities that shouldn’t cause pain, such as weight on your feet or blankets touching your skin, signals nerve damage.
Simple At-Home Tests to Identify Your Pain Source
Now that you recognize the symptoms, you can perform simple tests at home to confirm your pain source. These tests don’t require special equipment and take just a few minutes.
The pressure test for muscle pain
Apply firm pressure directly to the area where you feel discomfort. Muscle pain increases when you press on the affected spot. The tender point reproduces your symptoms, and you can pinpoint exactly where it hurts.
Press around the painful area using your fingers or thumb. The affected muscle feels sore to touch, and the pressure might be uncomfortable but shouldn’t cause sharp, shooting sensations. If pressing the area makes your pain worse in that specific spot without radiating elsewhere, you’re dealing with muscle involvement.
Acupressure points feel tender when stimulated, but the pressure shouldn’t hurt intensely. If light touch alone causes severe pain or the discomfort shoots down your arm or leg when you press, nerve issues may be present instead.
The movement test for joint pain
Joint pain shows distinct movement patterns. When you first wake up, your joints feel stiff and rigid. This morning stiffness typically eases within about 30 minutes as you move around.
Test your joint by moving it through its full range of motion. Bend, straighten, and rotate the affected area. Joint pain often limits how far you can move, and you might hear clicking or grinding sounds. The discomfort stays within the joint itself rather than spreading to surrounding areas.
Physical examination for musculoskeletal issues includes evaluation of range of motion as a key component. If movement gradually improves your symptoms after initial stiffness, joints are the likely source.
The tingling test for nerve pain
Tinel’s sign provides a simple way to check for nerve compression at home. Lightly tap with your fingertips over the area where you suspect nerve involvement. For example, tap the inside of your wrist if you think you have carpal tunnel syndrome, or tap behind your elbow for ulnar nerve issues.
A positive test produces tingling or a “pins and needles” sensation in the nerve’s distribution when you tap. You might feel the tingling shoot down into your fingers or toes. This indicates nerve compression or damage at that site.
The timing test: morning vs evening symptoms
Pain timing reveals important clues about its source. Morning joint pain presents as stiffness and lack of mobility due to reduced synovial fluid circulation during sleep. Evening joint pain feels achy and sore with burning or throbbing sensations caused by inflammation. Nerve pain often intensifies at night, manifesting as tingling or pins and needles.
What to Do for Each Type of Pain at Home
After identifying your pain source, the right home care approach can provide relief and speed recovery. Treatment strategies differ based on whether you’re dealing with muscle, joint, or nerve issues.
Managing muscle pain naturally
Muscle pain from minor injuries, stress, or exercise usually responds well to care at home. The RICE method works effectively: rest the affected area and take a break from activities that caused the injury, apply ice for 20 minutes three times daily, use compression with a stretchable bandage to reduce swelling, and elevate the injured area above your heart level to help gravity lessen inflammation.
Topical products containing menthol, lidocaine, or diclofenac sodium can ease discomfort when applied directly to sore muscles. Oral pain relievers such as acetaminophen, ibuprofen, or naproxen sodium provide additional relief. Begin mild stretching as your pain decreases to prevent stiffness.
Relieving joint stiffness and pain
Heat therapy offers temporary relief for aching joints. Apply heating pads, warm compresses, or soak in hot baths to increase blood circulation. For acutely inflamed joints, cold therapy with ice packs reduces swelling. Switch between heat and cold based on your symptoms.
Physical activity reduces joint pain and stiffness despite initial discomfort. Walking, swimming, water aerobics, and gentle yoga exercises improve flexibility without stressing joints. A diet rich in whole foods including fruits, vegetables, fish, nuts, and beans while avoiding processed foods helps manage inflammatory conditions. Weight loss significantly reduces arthritis pain, particularly for knee osteoarthritis.
Calming nerve pain symptoms
Warm baths increase blood circulation and decrease numbness symptoms. Regular exercise reduces blood sugar levels, which can slow nerve damage progression while increasing blood flow to extremities. Vitamin B complex (B1, B6, B12), vitamin E, and copper support nerve health. Turmeric contains anti-inflammatory properties that may offer pain relief.
Diluted essential oils like lavender, eucalyptus, or bergamot applied topically can reduce tingling sensations. Meditation techniques help lower stress and improve pain coping skills.
When home care isn’t enough
Seek medical attention if pain persists longer than a few weeks despite self-treatment. Severe pain that interferes with daily activities, sleep, or quality of life requires professional evaluation. Tingling in extremities indicates potential nerve damage that needs prompt assessment to prevent permanent complications. Pain accompanied by loss of mobility lasting more than a month warrants specialist consultation.
Warning Signs That Need Medical Attention
Some pain symptoms require professional evaluation rather than continued home treatment. Recognizing these warning signs helps you get timely care.
Signs of nerve compression pain
Nerve compression creates specific symptoms that distinguish it from other pain types. You’ll experience pain, numbness, or tingling around the compression site, usually at joints like your wrist, elbow, or ankle. Subsequently, you may notice an inability to move the affected area normally. Compression, inflammation, or injury to spinal nerve roots leads to shooting pain, weakness, numbness, or tingling in body parts along the nerve’s path.
Persistent pain that doesn’t improve
Chronic pain persists for three months or longer. If you rate your pain as seven or higher on a ten-point scale, comparable to a bad toothache, see a doctor immediately. Moderate pain that doesn’t resolve within a few days also warrants medical attention.
Weakness or loss of function
Sudden, severe muscle weakness requires emergency care. Weakness accompanied by warning signs can deteriorate rapidly, causing permanent disability. If pain limits your movement, work, or self-care abilities, a pain specialist can provide targeted treatment.
Night pain that disrupts sleep
More than half of patients with chronic pain experience sleep disorders. Two out of three people with chronic pain struggle with sleeping. Pain causes sleep maintenance insomnia, making it difficult to stay asleep throughout the night.
Conclusion
Identifying whether your pain comes from muscle, joint, or nerve doesn’t require a medical degree. Use the simple tests I’ve shared to pinpoint your discomfort source, and you’ll be able to apply the right treatment strategy from day one.
For one thing, accurate identification prevents you from wasting time on ineffective remedies. Muscle pain responds to rest and ice, while joint pain often improves with movement and heat. Nerve pain requires a different approach entirely.
If your symptoms persist beyond a few weeks or you notice warning signs like severe weakness or nighttime disruption, don’t hesitate to consult a healthcare professional for proper diagnosis and treatment.
Key Takeaways
Understanding the source of your pain enables you to choose the right treatment approach and avoid prolonging discomfort through ineffective remedies.
• Muscle pain feels dull and achy, worsens with direct pressure, and stays localized to the injury site • Joint pain causes morning stiffness that improves with movement and often includes grinding sensations • Nerve pain creates burning, shooting, or electric sensations that travel along nerve pathways • Simple at-home tests can identify pain source: pressure test for muscles, movement test for joints, tingling test for nerves • Seek medical attention for pain lasting over 3 weeks, weakness, or symptoms disrupting sleep
Each pain type requires different treatment strategies – muscle pain responds to rest and ice, joint pain improves with movement and heat, while nerve pain needs specialized care. Recognizing these distinctions helps you start effective treatment immediately rather than trying ineffective approaches.
FAQs
Q1. How can I tell if my pain is coming from a muscle or a nerve?
Muscle pain typically feels dull and achy, worsens when you press directly on the affected area, and stays localized to one spot. Nerve pain, on the other hand, feels like burning, shooting, or electric sensations that often travel along pathways in your body. Nerve pain may also cause tingling, numbness, or “pins and needles” feelings, which rarely occur with muscle issues.
Q2. What’s a simple way to test for nerve pain at home?
Try the tapping test: lightly tap with your fingertips over areas where you suspect nerve involvement, such as your wrist or elbow. If you feel tingling or a “pins and needles” sensation shooting down into your fingers or toes when you tap, this indicates possible nerve compression or irritation. Muscles don’t produce this buzzing response when tapped.
Q3. How does joint pain differ from nerve pain?
Joint pain typically causes stiffness, swelling, and aching sensations that are worst in the morning but improve with movement throughout the day. You might also hear grinding or clicking sounds. Nerve pain feels more like burning, tingling, or electric shocks that travel along nerve pathways and often worsen at night, frequently accompanied by numbness or weakness.
Q4. What are the key differences between muscle pain and joint pain?
Muscle pain presents as deep, tender discomfort that you can pinpoint to a specific spot and worsens when you press on it. Joint pain occurs where bones meet and causes stiffness, particularly in the morning, along with possible grinding sensations during movement. Joint pain tends to improve with gentle activity, while muscle pain typically requires rest.
Q5. When should I see a doctor for my pain instead of treating it at home?
Seek medical attention if your pain persists for more than three weeks despite home treatment, if you experience severe weakness or loss of function, if pain disrupts your sleep regularly, or if you notice tingling in your extremities. Pain rated seven or higher on a ten-point scale also warrants immediate professional evaluation.
Q6. How do I know if my pain is muscle, joint, or nerve?
Muscle pain is usually dull, sore, and tender to touch. Joint pain feels deep, stiff, and worse with movement or after rest. Nerve pain is sharp, burning, or electric-like, often with tingling or numbness and may travel along a path.
Q7. What does nerve pain feel like compared to muscle pain?
Nerve pain feels like shooting, burning, or electric shocks, sometimes with pins and needles or numbness. Muscle pain is more aching, tight, and localized, often increasing with activity or pressure.
Q8. Can I identify the type of pain at home?
Yes, you can get a good idea by observing:
- Location (localized vs radiating)
- Type (dull vs sharp/burning)
- Triggers (movement, rest, pressure)
This doesn’t replace a diagnosis but helps guide understanding.
Q9. Does nerve pain travel from one area to another?
Yes. Nerve pain often radiates along the nerve pathway, such as from the lower back to the leg (like sciatica) or from the neck to the arm.
Q10. Is pain that increases on pressing a muscle always muscular?
Most of the time, yes. Tenderness on pressing usually indicates muscle or soft tissue involvement, but sometimes deeper joint or trigger point issues can mimic this.
Q11. Why does my pain feel worse after rest?
Pain that worsens after rest is often joint-related (like early arthritis or stiffness). Muscles usually feel better after rest, unless they are very tight or injured.
Q12. What are the early signs of nerve compression?
Common early signs include:
- Tingling or “pins and needles”
- Numbness
- Burning or shooting pain
- Weakness in the affected limb
Q13. Is tingling always a sign of nerve damage?
Not always. Tingling can occur due to temporary nerve irritation or compression (like sitting awkwardly). Persistent or progressive tingling, however, should be evaluated.
Q14. Can muscle pain cause radiating symptoms?
Typically no. Muscle pain is usually localized, but trigger points can sometimes refer pain to nearby areas, which may mimic nerve pain.
Q15. When should I see a doctor for my pain?
Seek medical attention if you have:
- Persistent pain beyond a few weeks
- Severe or worsening symptoms
- Numbness, weakness, or loss of function
- Pain after injury or trauma
Consult for all the orthopedic related problems with Dr Manu Mengi

Dr. Manu Mengi is a best orthopedic doctor in Mohali, specializing in joint pain, arthritis, and sports injuries. With qualifications in orthopedics and advanced training in joint replacement, he provides effective care for bone and joint conditions, helping patients improve mobility and manage pain with the right treatment approach.