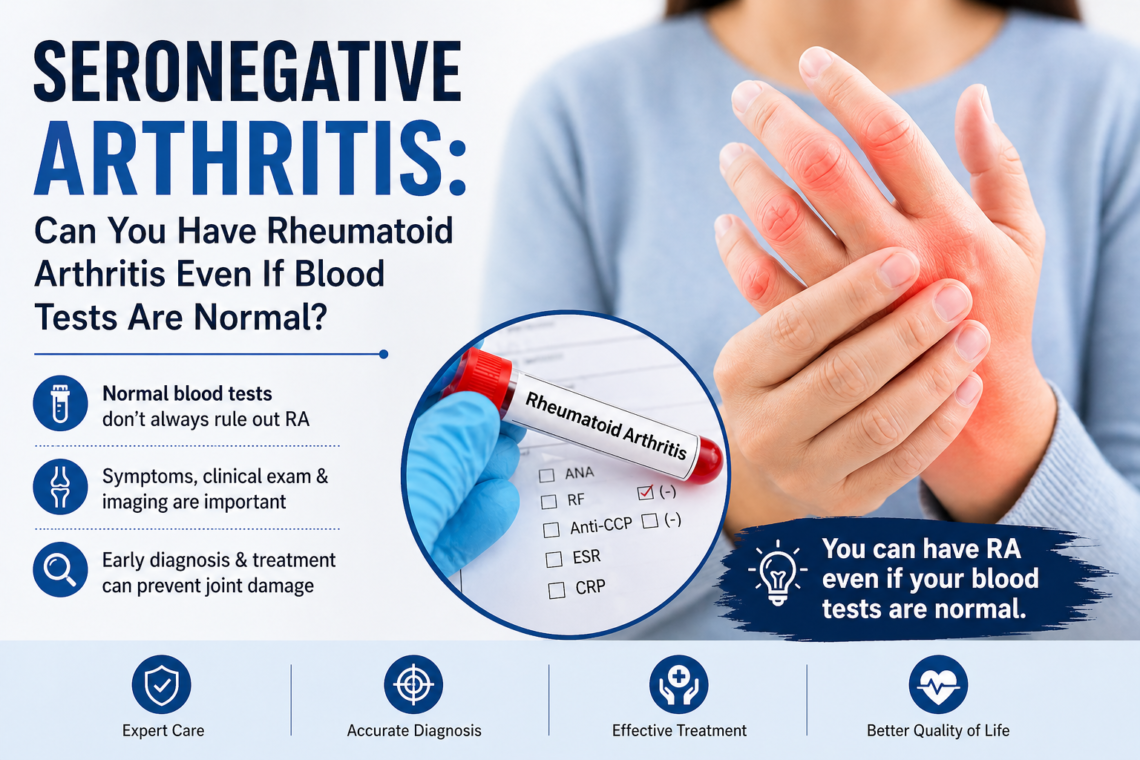
Can you have rheumatoid arthritis even if blood tests are normal? The answer might surprise you. In fact, about 15% to 20% of people with rheumatoid arthritis have negative rheumatoid factor (RF) test results. This condition is called seronegative rheumatoid arthritis, accounting for roughly 20% to 30% of all RA cases. Because standard blood tests don’t detect the usual antibodies in these patients, diagnosing seronegative RA requires a different approach. We’ll walk you through what seronegative rheumatoid arthritis is, how doctors diagnose it without positive blood tests, the key differences between seropositive and seronegative RA, and what treatment options are available for managing this form of inflammatory arthritis.
What Is Seronegative Rheumatoid Arthritis?
When you receive a diagnosis of rheumatoid arthritis but your blood work shows no signs of the typical antibodies, you have what doctors call seronegative rheumatoid arthritis. This form of RA presents the same joint pain and inflammation as the more common seropositive type, yet the standard markers simply don’t appear in blood tests.
Understanding rheumatoid factor and anti-CCP antibodies
Your immune system produces antibodies to protect you from infections and harmful invaders. Rheumatoid factor (RF) is a protein your immune system makes by mistake or when it becomes overactive. Unlike regular antibodies that fight germs, RF attacks healthy tissue in your body, particularly immunoglobulin G (IgG), one of your most common protective antibodies.
Anti-cyclic citrullinated peptide (anti-CCP) antibodies work similarly. These autoantibodies invade certain peptides in the lining of joints, triggering inflammation that leads to pain, swelling, and eventual joint damage. Around 60% to 80% of people diagnosed with RA test positive for anti-CCP. What makes anti-CCP particularly valuable for diagnosis is its specificity. Unlike RF, which appears in various conditions including hepatitis C, tuberculosis, and even in healthy older people[2], anti-CCP is very specific to rheumatoid arthritis.
Why blood tests come back negative
Several factors explain why your blood tests might not detect these antibodies. The levels of RF and anti-CCP vary considerably from person to person. If your levels are very low, standard blood tests simply won’t pick them up. In effect, you’re producing the antibodies, but in amounts too small for detection.
The timing of testing matters as well. Anti-CCP may be present in only 23% of people with early stage RA, increasing to 50% at diagnosis and 53% to 70% two years after diagnosis. This progression means early testing might miss antibodies that will appear later.
How common is seronegative RA
Seronegative RA accounts for approximately 20% to 30% of all rheumatoid arthritis cases. Between 60% and 80% of people diagnosed with RA test positive for rheumatoid factor, meaning the remaining 20% to 40% fall into the seronegative category.
While seronegative RA typically remains seronegative, changes can occur. Future blood tests sometimes reveal that rheumatoid factor has developed over time. However, it remains rare for someone who is seronegative to become seropositive.
How Is Seronegative Rheumatoid Arthritis Diagnosed?
Diagnosing seronegative rheumatoid arthritis requires more detective work than the seropositive form. Without positive antibody markers, doctors rely on clinical signs, inflammation markers, and imaging evidence to piece together an accurate diagnosis.
Symptoms doctors look for in seronegative RA
Your symptoms provide the first clues. Doctors assess whether you experience tenderness, swelling, and redness in your joints, particularly in the hands, knees, ankles, hips, and elbows. Morning stiffness lasting longer than 30 minutes signals inflammatory arthritis rather than ordinary joint wear.
The pattern matters just as much as the symptoms themselves. Persistent inflammation affecting joints on both sides of your body points toward RA rather than other conditions. Fatigue often accompanies these joint symptoms. Doctors also check for red or dry eyes, since RA can affect more than just your joints.
Physical examination findings
During your physical exam, doctors examine your joints for signs of synovitis, the hallmark of inflammatory arthritis. They look for swollen joints, particularly in your hands and feet, and assess how many joints show active inflammation. In reality, the number and pattern of affected joints heavily influence the diagnosis.
Blood tests that show inflammation
While RF and anti-CCP tests come back negative, other blood markers reveal inflammation. Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) levels indicate active inflammation in your body. ESR values correlate with radiological damage in seronegative RA. Normal acute phase reactants are infrequent in untreated RA and should prompt consideration of alternative diagnoses.
Imaging tests: X-rays, ultrasound, and MRI
X-rays detect erosion and damage to bone and cartilage. Seronegative RA shows more carpal fusion on hand and feet radiographs compared to seropositive RA. Ultrasound proves particularly useful, revealing a higher proportion of tenosynovitis in seronegative patients. MRI confirms diagnosis when physical examination cannot determine the presence of synovitis.
Diagnostic criteria used by rheumatologists
Rheumatologists use the ACR/EULAR classification criteria, which score various factors including joint involvement, serology results, acute-phase reactants, and symptom duration. Seronegative RA remains a clinical diagnosis that may take longer to confirm. Doctors must rule out conditions like psoriatic arthritis, ankylosing spondylitis, and osteoarthritis that produce similar symptoms.
Seropositive vs. Seronegative RA: Key Differences
The distinction between seropositive and seronegative RA extends beyond blood work. These two forms differ in severity, complications, and how they respond to specific medications.
Blood test results
Seropositive RA shows the presence of rheumatoid factor, anti-CCP antibodies, or both in blood tests. Between 60% and 80% of people with RA fall into this category. Seronegative RA means you don’t have these antibodies in your blood at all, or you don’t have much of them. RA seronegativity is defined as the absence of both RF and anti-CCP, while seropositivity requires at least one of the two antibodies.
Disease severity and progression
Seronegative RA has been considered a less severe disease subset than seropositive RA, with less radiographic damage. However, seropositive patients face significantly higher all-cause mortality with an odds ratio of 1.24. Kaplan-Meier analysis showed lower survival probabilities in the seropositive group at 76.51% versus 81.68%.
People with seropositive RA experience more extra-articular complications. They commonly develop firm lumps on or near affected joints called rheumatoid nodules, while seronegative patients generally don’t get these nodules. Seropositive patients show higher rates of vasculitis, inflamed blood vessels, rheumatoid lung issues, and cardiovascular disease. In contrast, interstitial lung disease occurs with an odds ratio of 2.42 in seropositive patients.
Risk of joint damage
During follow-up periods, 37.1% of 116 patients with seronegative RA showed radiographic damage. Seropositive patients had a higher risk of RA-related joint damage with an odds ratio of 1.24.
Response to treatment
Most medications work the same whether you’re seropositive or seronegative. However, seronegative patients may not respond as well to rituximab as seropositive patients. DMARD use was more frequent in seropositive patients. Because seronegative RA takes longer to diagnose, treatment delays might reduce your chances of achieving remission.
Treatment and Long-Term Outlook for Seronegative RA
Treatment for seronegative RA mirrors the approach used for seropositive disease. Your rheumatologist will prescribe medications from the same categories regardless of your antibody status.
Medications used to treat seronegative arthritis
NSAIDs like ibuprofen or naproxen reduce inflammation and pain during flare-ups. Corticosteroids manage severe symptoms but aren’t suitable for long-term use on account of adverse effects. Methotrexate serves as the first-line DMARD for most patients. Your doctor may add biologic DMARDs if methotrexate alone doesn’t control your symptoms. However, evidence suggests seronegative patients may not respond as well to rituximab compared to seropositive patients.
Importance of early treatment
Seronegative RA requires intensive treatment similar to seropositive RA. Starting methotrexate within three months of diagnosis more than doubles your chances of achieving a good or moderate therapeutic response. Basically, early intervention prevents joint damage and improves long-term outcomes.
Can seronegative RA become seropositive over time
About 13% of individuals with seronegative RA experience a change in diagnosis within 10 years. In similar fashion, 25% achieve drug-free remission during this period. While blood tests sometimes show rheumatoid factor development over time, this remains uncommon.
When to consider getting a second opinion
Seek another rheumatologist’s perspective if your diagnosis remains unclear, your current treatment isn’t working, or you’re facing major treatment decisions. Second opinions are common in rheumatology and provide peace of mind.
Conclusion
Seronegative rheumatoid arthritis proves you don’t need positive blood tests to have RA. While diagnosing this condition requires more detective work from your rheumatologist, the treatment approach remains equally effective. Undoubtedly, early intervention with DMARDs gives you the best chance at managing symptoms and preventing joint damage. If you’re experiencing persistent joint pain and swelling despite negative antibody tests, don’t dismiss the possibility of seronegative RA. Work closely with your rheumatologist to get the right diagnosis and treatment plan.
Key Takeaways
Understanding seronegative rheumatoid arthritis can help you recognize that normal blood tests don’t rule out RA, and proper diagnosis and treatment remain crucial for joint health.
• You can have RA with normal blood tests – 20-30% of RA cases are seronegative, meaning standard antibody tests (RF and anti-CCP) come back negative despite active disease.
• Diagnosis relies on clinical evidence – Doctors use joint swelling patterns, inflammation markers (ESR/CRP), imaging tests, and physical symptoms rather than antibody results.
• Seronegative RA is generally less severe – Patients typically experience fewer complications, less joint damage, and better survival rates compared to seropositive cases.
• Early treatment is critical for both types – Starting methotrexate within three months doubles your chances of good therapeutic response, regardless of antibody status.
• Most treatments work equally well – Standard RA medications like methotrexate and biologics are effective for seronegative patients, though rituximab may be less responsive.
The key message: Don’t let negative blood tests delay proper evaluation if you have persistent joint symptoms. Seronegative RA requires the same aggressive treatment approach as seropositive disease for optimal outcomes.
FAQs
Q1. Can I have rheumatoid arthritis even if my blood tests come back normal?
Yes, you can have rheumatoid arthritis with normal blood test results. This is called seronegative RA, and it accounts for about 20-30% of all rheumatoid arthritis cases. While standard antibody tests (RF and anti-CCP) may be negative, you can still have active disease with joint inflammation and pain.
Q2. What does “seronegative” actually mean?
“Seronegative” simply means that commonly used blood markers like RF and anti-CCP are not detected in the blood, even though the disease process may still be present.
Q3. What are the early symptoms of seronegative rheumatoid arthritis?
Early signs often include:
- Morning stiffness
- Pain and swelling in small joints (hands, wrists, feet)
- Fatigue
Difficulty making a fist or gripping objects
Q4. How is rheumatoid arthritis diagnosed without positive blood tests ?
Diagnosis is clinical. It is based on:
- Persistent joint pain and swelling
- Morning stiffness (typically >30–60 minutes)
- Symmetrical joint involvement
Imaging (X-ray, ultrasound, MRI)
Blood tests support the diagnosis, but they are not mandatory.
Q5. How do doctors diagnose seronegative rheumatoid arthritis without positive antibody tests?
Doctors diagnose seronegative RA by examining your symptoms, conducting physical examinations of your joints, checking for inflammation markers like ESR and CRP, and using imaging tests such as ultrasound, X-rays, or MRI. They look for patterns of joint swelling, morning stiffness lasting over 30 minutes, and inflammation affecting both sides of your body.
Q6. Is seronegative RA less severe than seropositive RA?
Generally, seronegative RA is considered less severe than seropositive RA. People with seronegative disease typically experience less joint damage, fewer extra-articular complications like rheumatoid nodules, and better survival rates. However, both types require early and aggressive treatment to prevent progression.
Q7. Will the same medications work for seronegative rheumatoid arthritis?
Most RA medications work equally well for both seronegative and seropositive patients. Methotrexate is typically the first-line treatment, and biologic DMARDs can be added if needed. The main exception is rituximab, which may not be as effective for seronegative patients compared to those who are seropositive.
Q8. Can seronegative RA change to seropositive over time?
While it’s possible for seronegative RA to become seropositive, this is uncommon. About 13% of people with seronegative RA may experience a change in diagnosis within 10 years, and blood tests may occasionally show rheumatoid factor development later. However, most people who are seronegative remain seronegative throughout their disease course.
Q9. Can my blood tests become positive later ?
Yes. Some patients initially test negative but may become seropositive over time as the disease evolves.
Q10. Which tests help when blood reports are normal?
Imaging plays a key role:
- Ultrasound can detect early synovitis
MRI can show inflammation before X-rays
These help confirm inflammation when blood tests are inconclusive.
Q11. What conditions can mimic seronegative rheumatoid arthritis?
Several conditions can look similar, including:
- Osteoarthritis
- Psoriatic arthritis
- Ankylosing spondylitis
- Viral arthritis
- Lupus
Proper evaluation is essential to avoid misdiagnosis.
Q12. Should I delay treatment if my reports are normal?
No. If clinical suspicion is high, early treatment is crucial. Waiting for blood tests to turn positive can delay care and increase the risk of joint damage.
Q13. Is treatment different for seronegative rheumatoid arthritis?
The treatment principles are the same as seropositive RA:
Lifestyle modifications
DMARDs (like methotrexate)
Physiotherapy
The goal remains early control of inflammation and prevention of joint damage.

Dr. Manu Mengi is a best orthopedic doctor in Mohali, specializing in joint pain, arthritis, and sports injuries. With qualifications in orthopedics and advanced training in joint replacement, he provides effective care for bone and joint conditions, helping patients improve mobility and manage pain with the right treatment approach.