Rotator Cuff Tear vs. Frozen Shoulder | Dr. Manu Mengi
Rotator Cuff Tear vs. Frozen Shoulder confusion is something I encounter frequently in my practice, with many patients mistakenly self-diagnosing their shoulder pain. These two conditions are often confused with each other, yet they present distinct symptoms and have significantly different recovery timelines.
In my experience, understanding the key differences can help you identify your condition more accurately. Rotator cuff tears typically have a sudden onset, particularly after activities like lifting something heavy or falling. At the same time, frozen shoulder develops gradually with pain that slowly worsens over weeks or months. The most telling difference? If you have a rotator cuff tear, you can likely lift your shoulder without assistance. However, with a frozen shoulder, you’ll face difficulty raising your arm by yourself.
Throughout this guide, I’ll walk you through the specific symptoms, causes, and treatments for both conditions. We’ll explore why frozen shoulder involves progressive stiffness accompanied by dull, aching pain (especially at night), while rotator cuff tears cause sharper, more localised pain when lifting or rotating the arm. By the end, you’ll understand why that stiffness in your shoulder joint might indicate one condition over the other.
This self-diagnosis often leads to anxiety. If you're in Mohali and struggling with shoulder pain, the most important step is to get a professional evaluation. Book an appointment with a specialist to get an accurate diagnosis and peace of mind.
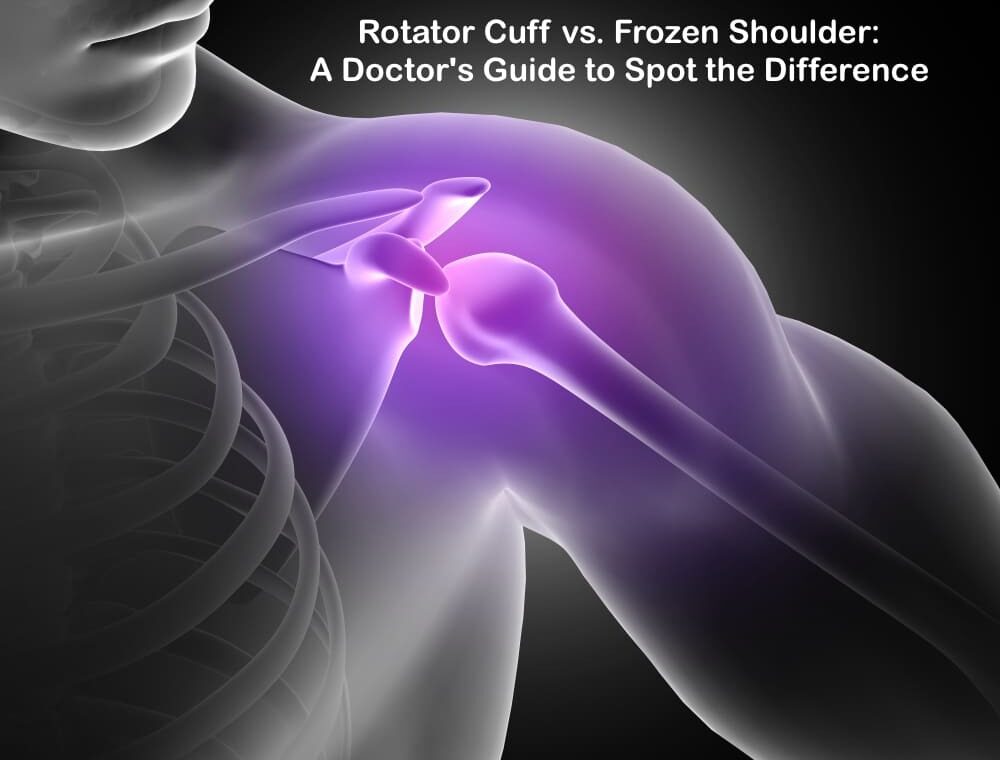
Understanding the Shoulder: Anatomy and Function
The shoulder represents one of the most complex and mobile joints in the human body. To fully understand the differences between rotator cuff injuries and frozen shoulder, we must first examine the intricate architecture that allows for this remarkable range of motion. Unlike other joints that prioritise stability, the shoulder sacrifices some stability for mobility, making it uniquely susceptible to certain conditions.
The role of the rotator cuff in shoulder movement
The rotator cuff forms the cornerstone of shoulder function – a group of four muscles and their tendons that surround the shoulder joint like a protective collar. This muscular quartet connects your shoulder blade (scapula) to your upper arm bone (humerus) and works together to enable precise movement while maintaining joint stability.
The four muscles that make up this critical structure include:
- Supraspinatus: Initiates the first 15 degrees of arm abduction (lifting your arm away from your body)
- Infraspinatus: Powers external rotation of the arm away from your body
- Teres minor: Assists with external rotation and stabilisation
- Subscapularis: Enables internal rotation (turning your arm toward your body)
A helpful mnemonic for remembering these muscles is “SITS” – Supraspinatus, Infraspinatus, Teres minor, and Subscapularis.
The primary biomechanical role of these muscles extends beyond their movement function. They compress the head of the humerus against the shallow glenoid cavity of the scapula, creating what doctors call “dynamic stability”. Without this muscular support, the disproportionate size between the humeral head and the glenoid fossa (a 4:1 surface area ratio) would make the joint highly unstable.
Furthermore, these muscles don’t work in isolation. For example, during abduction, the supraspinatus handles the initial 0-15 degrees of movement, then the deltoid muscle takes over from 15-90 degrees. Finally, the scapula must rotate to achieve full range of motion, which is accomplished by the trapezius and serratus anterior muscles.
What is the shoulder capsule, and why does it matter
Surrounding the glenohumeral joint is a fibrous sheath called the shoulder capsule. This structure extends from the anatomical neck of the humerus to the rim of the glenoid fossa, completely enveloping the joint. Unlike other joint capsules in your body, the shoulder capsule has a unique characteristic – it’s remarkably loose and lax, allowing the bones to separate by more than 2.5 cm.
This laxity isn’t a design flaw but rather a deliberate feature that permits the extensive freedom of movement characteristic of the shoulder joint. Nevertheless, this same feature also makes the joint more vulnerable to instability and injury.
The capsule doesn’t work alone in providing joint stability. It’s reinforced by:
- The glenoid labrum – a fibrocartilaginous ring that deepens the glenoid cavity
- Ligaments that connect bones to bones
- Tendons that connect muscles to bones
- The rotator cuff muscles themselves, which fuse with the capsule
Additionally, fluid-filled sacs called bursae surround the capsule, facilitating smooth movement by reducing friction between the structures. The synovial membrane inside the capsule produces lubricating fluid that further aids motion.
Interestingly, when the shoulder capsule becomes damaged or inflamed, it can lead to adhesive capsulitis – commonly known as frozen shoulder. In this condition, the capsule thickens and becomes stiff, significantly restricting movement and causing pain.
How shoulder mobility is affected by injuries
Given the complexity of the shoulder’s structure, it’s not surprising that injuries can substantially impact its function. Shoulder pain affects approximately 18 million Americans each year, with rotator cuff tears accounting for a significant number of these cases.
Rotator cuff tears can occur through trauma, overuse, or age-related degeneration. These tears affect one in every four adults aged 60 years and older, with the supraspinatus tendon being most commonly involved. Risk factors include smoking, high cholesterol, and family history.
When the rotator cuff is damaged, patients typically experience:
- Pain during overhead activities
- Limited range of motion
- Weakness in the shoulder
- Difficulty with daily activities
Studies using three-dimensional motion analysis have shown that individuals with symptomatic rotator cuff tears exhibit abnormal shoulder motion when performing common daily tasks compared to those without tears. This dysfunction occurs because rotator cuff injuries compromise the joint’s dynamic stability, creating muscle force imbalances.
Alternatively, when the shoulder capsule becomes inflamed and thickened in adhesive capsulitis (also known as frozen shoulder), patients experience progressive stiffness and significant pain. This condition not only limits one movement but can also restrict motion in multiple directions simultaneously.
Research shows that patients with rotator cuff-related shoulder pain demonstrate significantly less shoulder flexion, internal and external rotation range of motion compared to individuals without shoulder problems. This finding helps explain why these conditions have such a profound impact on everyday activities.
Both conditions can make simple tasks challenging – whether reaching for objects on high shelves, putting on a coat, or even combing your hair. Understanding the underlying anatomy helps explain why these different conditions can sometimes present with similar symptoms despite having distinct causes.
As we've seen, both conditions severely impact your daily life. The key to effective treatment is a correct diagnosis. If you're experiencing limited motion or pain, consider visiting a
Specialised Shoulder Clinic in Mohali for a comprehensive assessment.
Rotator Cuff Tear: Causes, Symptoms, and Diagnosis
Rotator cuff tears represent one of the most common shoulder injuries I diagnose in my practice. These tears are the leading cause of shoulder pain and shoulder-related disability, affecting millions of people each year. In fact, more than 2 million Americans experience some rotator cuff problem annually. While these injuries can affect people of all ages, they’re particularly common in adults over 40, with prevalence increasing significantly with age.
As a physician, I find that many patients are surprised to learn that some individuals have rotator cuff tears without experiencing any symptoms whatsoever. This silent presentation can make diagnosis challenging in certain cases.
Common causes: trauma, overuse, and ageing
Rotator cuff tears typically fall into two distinct categories: acute traumatic tears and degenerative tears. Understanding this distinction is crucial for proper treatment.
Traumatic (Acute) Tears occur suddenly as a result of a specific injury. In my experience, patients often report:
- Falling on an outstretched arm
- Lifting something heavy with a jerking motion
- Experiencing sudden force while pushing or pulling
- Sustaining an injury during a shoulder dislocation
These traumatic tears account for approximately 8% of all rotator cuff injuries. They tend to stem from higher energy mechanisms and typically cause full-thickness tears, whereas degenerative tears often begin as partial-thickness injuries. Moreover, traumatic tears generally are larger and more likely to involve the subscapularis muscle.
Degenerative (Wear-Related) Tears develop gradually over time due to natural ageing processes. These constitute the majority of rotator cuff injuries I see in my practice. Several factors contribute to these tears:
- Repetitive stress – Certain activities that involve repeated shoulder motions put significant strain on the rotator cuff. Sports like baseball, tennis, rowing, and weightlifting carry an increased risk of overuse. Likewise, many occupations requiring repetitive overhead movements can lead to progressive damage.
- Decreased blood supply – As we age, blood flow to our rotator cuff tendons diminishes. Without adequate blood supply, the body’s natural ability to repair tendon damage becomes impaired, ultimately leading to tissue breakdown.
- Bone spurs, also known as age-related bone overgrowth (osteophytes), can develop on the acromion, creating friction against the rotator cuff tendons when you move your arm.
Essentially, the supraspinatus tendon bears the brunt of most rotator cuff injuries, as it endures the majority of shoulder-stabilising strain. Approximately 53% of patients with supraspinatus tears also have involvement of the infraspinatus.
Concerning symptoms, patients typically experience:
- Pain localised to the anterior shoulder or greater tuberosity area
- Discomfort when lying on the affected shoulder
- Pain with overhead activities
- Night pain that interrupts sleep
- Weakness in the affected arm
- Crackling or popping sensations during certain movements
- A positive painful arc sign during clinical examination
Diagnosing rotator cuff tears involves several components. First, I take a detailed history, including the mechanism of injury and activities that aggravate or relieve symptoms. Next, I perform a thorough physical examination, checking for tenderness, range of motion, and specific clinical tests designed to stress the rotator cuff tendons. Additionally, diagnostic imaging plays a crucial role in confirming the diagnosis and determining the extent.
Specifically, when patients present with an inability to elevate their arm after a traumatic event, despite normal radiographs, I maintain a high index of suspicion for rotator cuff pathology, as these injuries can often be missed during initial assessment.
While this guide helps you understand the differences, only a physical examination can confirm your condition. For expert rotator cuff tear treatment in Mohali or frozen shoulder treatment in Mohali, seeking help from a qualified orthopaedic doctor is crucial. Learn more about your Shoulder Pain Treatment Options in Mohali.
Key Takeaways
Understanding the differences between rotator cuff tears and frozen shoulder can help you identify your condition and seek appropriate treatment more effectively.
• Onset patterns differ significantly: Rotator cuff tears typically occur suddenly after trauma or lifting, while frozen shoulder develops gradually over weeks to months with progressively worsening pain.
• Movement ability is the key differentiator: With rotator cuff tears, you can usually lift your arm without assistance, but frozen shoulder severely limits your ability to raise your arm independently.
• Pain characteristics vary between conditions: Rotator cuff tears cause sharp, localised pain during lifting or rotation, while frozen shoulder presents as dull, aching pain that’s particularly troublesome at night.
• Age and activity patterns matter for diagnosis: Rotator cuff tears affect over 25% of adults aged 60+, often from repetitive overhead activities or sudden trauma. At the same time, a frozen shoulder involves inflammation and stiffness of the capsule.
• The rotator cuff’s four muscles (SITS) – Supraspinatus, Infraspinatus, Teres minor, and Subscapularis – work together to provide dynamic shoulder stability, making tears particularly disabling for daily activities.
Both conditions significantly impact quality of life; however, accurate identification of symptoms, such as pain location, movement limitations, and onset patterns, enables more targeted treatment approaches and better outcomes.
FAQs
Q1. How can I differentiate between a frozen shoulder and a rotator cuff tear?
A1. The key difference lies in your ability to move your arm. If you can lift your arm independently, it’s more likely to be a rotator cuff tear. Frozen shoulder severely limits your ability to raise your arm without assistance. Additionally, rotator cuff tears often have a sudden onset, while frozen shoulder develops gradually over time.
Q2. Is it possible for a rotator cuff tear to be misdiagnosed as frozen shoulder?
A2. Yes, these conditions can be confused. Some partial rotator cuff tears may not cause pain and can mimic symptoms of a frozen shoulder. However, a thorough medical examination, including imaging tests, can help differentiate between the two conditions.
Q3. What are the most effective treatments for frozen shoulder?
A3. Most cases of frozen shoulder improve on their own within 12 to 18 months. For severe or persistent symptoms, treatments may include physical therapy, corticosteroid injections, and in some cases, surgery. Steroid injections can be particularly effective when administered early in the progression of the condition.
Q4. What other conditions can be mistaken for a rotator cuff tear?
A4. Several shoulder conditions can present similar symptoms to rotator cuff tears, including biceps tendinitis, shoulder impingement syndrome, labral tears, arthritis, bursitis, and tendinitis. Each of these conditions affects different parts of the shoulder structure but may cause similar pain or movement limitations.
Q5. How does age affect the likelihood of developing rotator cuff tears?
A5. The risk of developing a rotator cuff tear increases significantly with age. They are particularly common in adults over 40, with more than 25% of adults aged 60 and older experiencing some form of rotator cuff tear. This is often due to natural wear and tear, decreased blood supply to the tendons, and the development of bone spurs that can irritate the rotator cuff over time.
Still unsure about your shoulder pain? Don't let it limit your life any longer. If you're looking for an Affordable Shoulder Treatment in Mohali or simply want to consult with a trusted expert, reach out to us today. Schedule a consultation to get a clear diagnosis and start your journey to recovery.
📞 Call Us: +91 87250 11661 | 📍 Find Our Clinic: Google My Business
📖 Learn More About Shoulder Pain:
- Frozen Shoulder
- Shoulder Pain: Exploring Causes and Treatment
- Why Your Shoulder Joint Pain Won’t Go Away: Expert Guide to Relief
- Rotator Cuff Injuries: Symptoms, Diagnosis and Treatment Options
Dr. Manu Mengi – Shoulder Pain Specialist in Mohali
With extensive experience in diagnosing and treating complex shoulder conditions, Dr. Manu Mengi is a leading Shoulder Pain Specialist in the Mohali and Tricity region. He is dedicated to providing personalised care, utilising accurate diagnosis and evidence-based treatment plans to help patients regain pain-free movement and improve their quality of life.

Dr. Manu Mengi is a best orthopedic doctor in Mohali, specializing in joint pain, arthritis, and sports injuries. With qualifications in orthopedics and advanced training in joint replacement, he provides effective care for bone and joint conditions, helping patients improve mobility and manage pain with the right treatment approach.


 Want a personalised joint-friendly workout plan? Visit the
Want a personalised joint-friendly workout plan? Visit the  Rated 5/5 on Google:
Rated 5/5 on Google:  +91 87250 11661 |
+91 87250 11661 |  SCO-41, Sector 80
SCO-41, Sector 80











